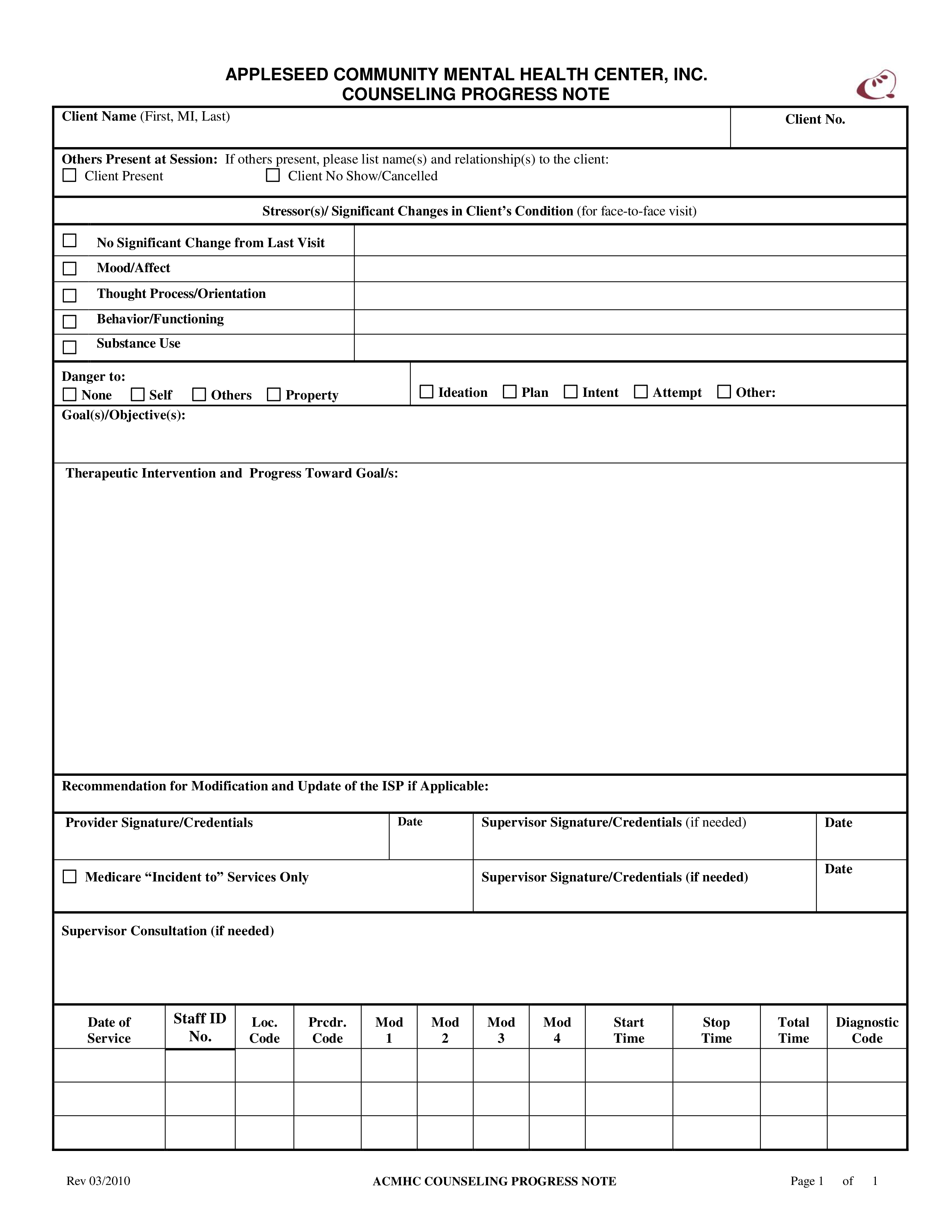

The process of effective counseling often hinges on meticulous record-keeping. Accurate and detailed notes are crucial for maintaining continuity, facilitating collaboration with other professionals, and providing a valuable resource for the client. A well-structured Counseling Progress Notes Template is an invaluable tool for any therapist or counselor. It's more than just a log; it's a communication tool designed to capture key information, track progress, and inform treatment decisions. This article will delve into the essential components of a robust Counseling Progress Notes Template, exploring its purpose, structure, and best practices. Counseling Progress Notes Template – understanding its significance is the first step towards providing truly effective care.
The core function of a Counseling Progress Notes Template is to systematically document a client's interactions and progress throughout a session or period. It's a standardized format that encourages clear, objective reporting, minimizing subjective interpretations and promoting consistency across different providers. Without a consistent and detailed record, it becomes difficult to assess the client's needs, monitor treatment effectiveness, and ensure continuity of care. A thoughtfully designed template empowers practitioners to proactively address challenges, celebrate successes, and tailor interventions to meet individual client goals. It's a vital component of ethical and professional practice.

Understanding the Purpose of a Counseling Progress Notes Template
Before diving into the specifics, it's important to understand why a Counseling Progress Notes Template is so important. It serves several key purposes:

- Documentation: It provides a permanent record of the client's experience, allowing for future reference.
- Collaboration: It facilitates communication with other members of the treatment team – psychiatrists, social workers, psychologists, and other specialists.
- Treatment Planning: The notes inform the development of a comprehensive treatment plan, outlining goals, interventions, and expected outcomes.
- Client Self-Reflection: The notes can be a valuable tool for the client to reflect on their experiences and identify patterns in their behavior or emotions.
- Billing and Insurance: Many insurance companies and billing practices require detailed documentation of client sessions.
The template isn't meant to be a rigid, pre-determined form. It's a flexible framework that can be adapted to suit the specific needs of each client and treatment approach. The key is to ensure that the notes are clear, concise, and objective.

The Essential Sections of a Counseling Progress Notes Template
Let's examine the key sections typically included in a comprehensive Counseling Progress Notes Template. Each section contributes to a holistic understanding of the client's journey.

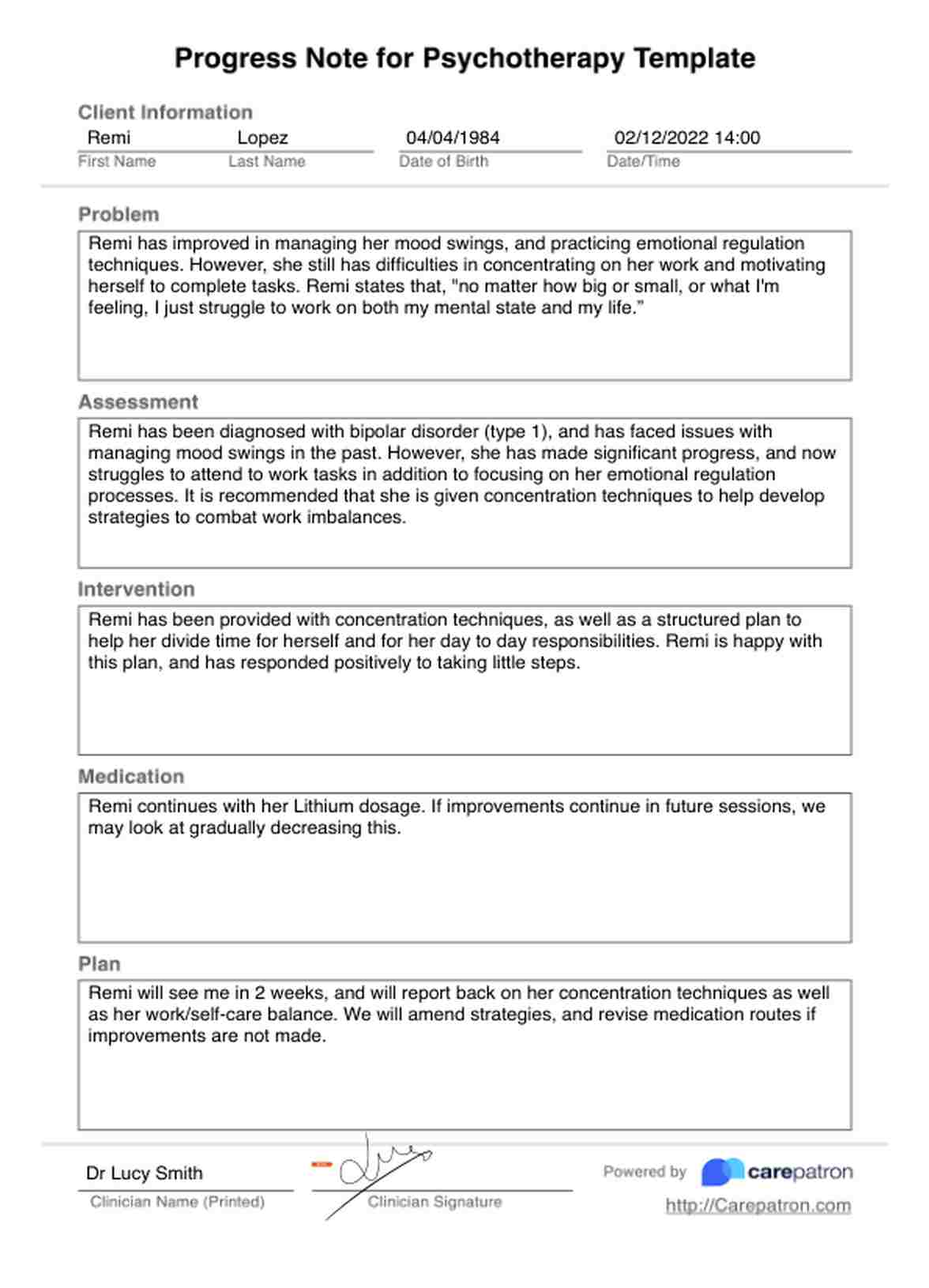
1. Client Demographics & Session Details
This initial section gathers basic information about the client, including:

- Client's Full Name
- Date of Birth
- Contact Information (phone, email)
- Session Number
- Type of Session (e.g., individual, group, family)
2. Session Summary
This is the heart of the template, providing a brief overview of the session's key events. It should be concise and focused on the most important points.

- Date and Time of Session
- Client's Initial Statement/Problem (briefly summarize the client's primary concern)
- Key Topics Discussed (list 3-5 major topics covered)
- Client's Reactions/Emotions (note any noticeable shifts in the client's demeanor)
3. Assessment & Observations
This section focuses on the client's current state and any relevant assessments made during the session.
- Mental Status Examination (MSE) Observations: Describe any notable observations regarding the client's presentation (e.g., mood, affect, thought processes, cognitive functioning).
- Behavioral Observations: Note any specific behaviors exhibited by the client (e.g., restlessness, withdrawal, increased activity).
- Emotional Assessment: Document the client's emotional state – are they experiencing anxiety, sadness, or other emotions?
- Relevant Data Collected: Include any standardized assessments used (e.g., Beck Depression Inventory, GAD-7).
4. Treatment Plan Integration
This section demonstrates how the session's content aligns with the client's goals and treatment plan.

- Goals Revisited: Review the client's stated goals and assess whether they are being addressed.
- Interventions Used: Detail the specific interventions employed during the session (e.g., cognitive restructuring, relaxation techniques, motivational interviewing).
- Progress Towards Goals: Note any progress made towards achieving the client's goals.
- Adjustments to the Plan: Document any modifications to the treatment plan based on the client's response.
5. Client Reflections & Progress
This section allows the client to reflect on their experience and provide feedback.

- Client's Perspective: Record the client's own assessment of their experience during the session.
- Client's Feelings: Document the client's emotional response to the session.
- Client's Self-Reported Progress: Ask the client about their perceived progress in addressing their concerns.
- Client's Strengths: Note any strengths or positive aspects of the client's experience.
6. Homework & Next Steps
This section outlines any tasks assigned to the client and the anticipated follow-up.
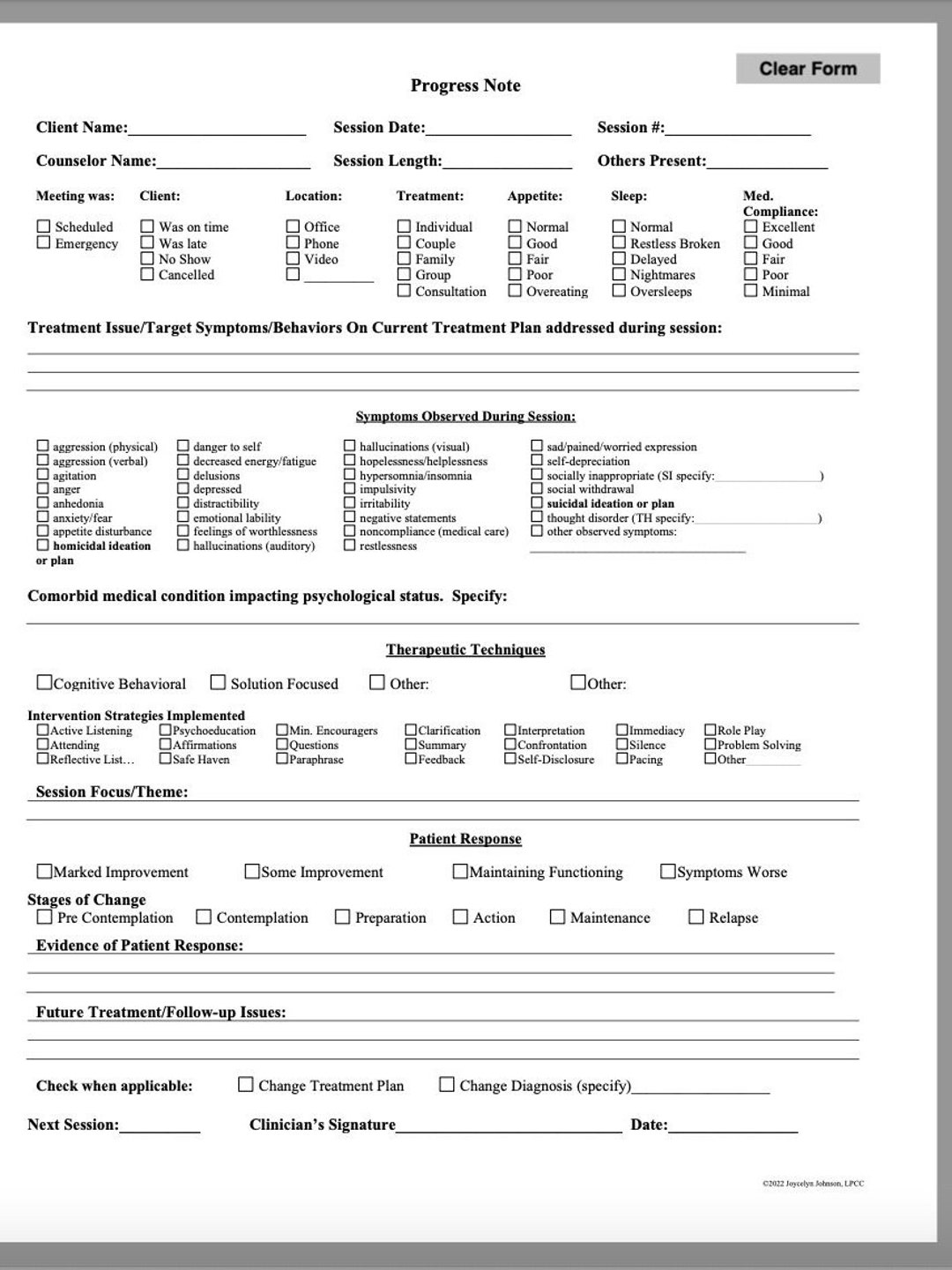

- Homework Assignments: Specify any homework assignments (e.g., journaling, relaxation exercises, behavioral experiments).
- Follow-Up Appointments: Schedule any scheduled follow-up appointments.
- Resources Provided: List any resources provided to the client (e.g., websites, support groups).
Conclusion
Counseling Progress Notes Templates are an indispensable tool for effective therapy. By providing a structured and detailed record of client interactions, these templates empower practitioners to maintain continuity of care, facilitate collaboration, and ultimately, contribute to the client's successful treatment. The consistent application of a well-designed template is a cornerstone of ethical and professional practice. Remember that the template is a guide, not a rigid rulebook. Flexibility and adaptation are key to ensuring that the notes accurately reflect the client's experience and contribute to positive outcomes. Ultimately, the goal is to build a strong therapeutic relationship based on trust, transparency, and a shared commitment to client well-being. Counseling Progress Notes Template – utilizing this template effectively is a demonstration of commitment to client-centered care.
0 Response to "Counseling Progress Notes Template"
Posting Komentar